At Hand to Shoulder Center of Wisconsin, our orthopedic doctors and specially trained staff have extensive experience treating tennis elbow. Learn more about tennis elbow treatments and exercises and how the orthopedic team of specialists at Hand to Shoulder Center of Wisconsin can help.
What is Tennis Elbow?
Lateral epicondylitis, more commonly known as tennis elbow, is described as degenerative changes that occur at the common extensor tendon. The common extensor tendon attaches to the lateral epicondyle of the elbow. Pain associated with this diagnosis is most commonly located on the outside area of the elbow.
What causes Tennis Elbow and what structure(s) are injured?
The exact cause of lateral epicondylitis is unknown; however, it is commonly caused by repetitive overuse of the wrist extensor muscles. This condition can be associated with micro tears of the muscles/tendons, tendinitis, arthritis of the underlying joint, as well as decreased blood flow that can cause weakness and damage to the fibrous portion of the tendons. Continued micro trauma to the wrist extensors with repetitive use inhibits proper healing and may continue to damage the tissue.
Men are more likely to develop lateral epicondylitis and it has been found to be more common with patients in their late 30’s to 40’s.
What are the symptoms of Tennis Elbow?
Lateral epicondylitis or tennis elbow presents with pain located along the outside area of the elbow. Sometimes this pain can radiate down into the forearm to the back of the hand. Patients may report that pain increases with bending the wrist forward and straightening the elbow as well as night time aching and morning stiffness. Difficulty can occur with grasping, holding, and gripping objects.
How is Tennis Elbow diagnosed?
The diagnosis of lateral epicondylitis is found through a thorough examination by a trained health care provider. At Hand to Shoulder Center of Wisconsin, this examination is completed by a hand and upper extremity fellowship-trained orthopedic physician. Our physician will inquire about the past medical history, medications, current symptoms and health status, social history, occupation, and recreational activities. A physical examination is also completed and manual testing is done to identify the presence of lateral epicondylitis.
No imaging or lab studies are required to diagnose tennis elbow. An x-ray may be ordered to rule out other conditions and sometimes, a MRI may be performed to rule out ligamentous injury.
How to treat Tennis Elbow?
Lateral epicondylitis is managed initially by using the “PRICE” principle: Protection, Rest, Ice, Compression, and Elevation. Pain is best managed by avoidance of all activities that are noted to aggravate the injured area.
At Hand to Shoulder Center of Wisconsin the physician may refer the patient to a licensed physical or occupational therapist for conservative care of their symptoms. Once referred to a therapist, many forms of intervention are initiated and can include stretches, strengthening, soft tissue massage, other manual techniques, modalities, and splinting (Fig. 1-4). All exercises target flexibility and increased strength with use of functional activities. The therapist may choose to use a modality as a treatment option to control the patient’s pain. Modalities that are commonly used include ultrasound and iontophoresis.
 Figure 1: Forearm stretch |
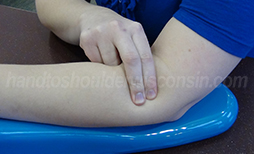 Figure 2: Cross friction massage |
 Figure 3: Specific strengthening of wrist extensors |
 Figure 4: Specific strengthening of wrist extensors |
On occasion, the therapist may recommend a resting splint to relieve the tension of the involved muscles/tendons. This orthotic/splint may be pre-fabricated or custom made. Another option for splinting may be the use of a counter-force brace or “tennis elbow strap”. This brace redistributes the forces of the muscles/tendons (Fig. 5). With use of the Tennis Elbow brace it is important to understand that nerve symptoms may occur if the brace is too tight. These symptoms can include numbness and tingling into the back portion of the forearm into the hand.

Figure 5: Tennis elbow strap
In severe cases of lateral epicondylitis, surgery may be warranted. At Hand to Shoulder Center of Wisconsin, tennis elbow surgery is performed as an outpatient procedure and varies between open surgical and arthroscopic techniques. Postoperative, the patient attends therapy and a specific treatment plan is designed by a physical or occupational therapist to best fit the patient’s needs.
**Ensure all exercises are performed without pain