Hand to Should Center has an experienced team of orthopedic doctors that are here to diagnose and treat your severe hand pain. Contact Hand to Shoulder Center of Wisconsin in Appleton or Green Bay, WI today to learn more about how our orthopedic specialists and therapists can help you.
De Quervain’s tenosynovitis is a condition that affects the tendons in the wrist and the base of the thumb. It develops when the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons around the base of the thumb become swollen, often causing inflammation to develop. This condition affects the lining of the tendon sheaths that surrounds the tendons. It is often painful and affects the patient’s ability to move the thumb and is especially painful when the tendons and sheaths are placed in a stretched position.
Tendons are flexible, rope-like tissue that connects muscle to bone. Muscles pull on the APL and EPB tendons located on the back of the forearm to promote thumb movement.
De Quervain’s Tenosynovitis Symptoms and Causes
In de Quervain’s tenosynovitis, the symptoms typically occur gradually and with certain activities, especially grasping and pinching. The most common symptoms are soreness and the inability to move your thumb freely without pain. Other associated symptoms often include:
- Tenderness and thumb pain
- Wrist pain and/or redness of the wrist at the base of the thumb
- Forearm pain on the thumb side
- Soreness and thumb swelling
- Difficulty or the inability to pinch or grasp items
The cause of de Quervain is unknown. However, repeatedly performing repetitive motions such as pinching and squeezing may lead to swelling and inflammation, causing pain in the wrist or thumb. Sports, such as golfing and tennis or work related activities that involve repetitive wrist flexion and extension can also cause pain in the hand (thumb region) that may be associated with de Quervain’s. This is a common condition found in new mothers, due to the awkward thumb positions with supporting a newborn baby.
Typically de Quervain is more common in females between 30-50 years of age. Conditions like rheumatoid arthritis can also increase the chances of developing tenosynovitis. Social habits from the overuse of your texting thumbs may play a role in causing inflammation. Certain medical conditions such as diabetes, alcoholism, cirrhosis of the liver, and seizure disorders appear to also increase the chances of developing de Quervains.
De Quervain’s Tenosynovitis Diagnosis and Treatment
At Hand to Shoulder Center of Wisconsin, our subspecialty trained hand surgeons conduct a thorough examination. All prior hand, wrist, and arm injuries and conditions are reviewed along with performing a visual and physical examination of the upper extremity and hand. Close attention is paid to the location of the pain. Often a Finkelstein Test is used to aid in diagnosing de Quervain tenosynovitis.
A Finkelstein Test is a non-complex test that involves making a fist with your thumb tucked into your palm. The wrist is then bent towards the pinky side. If pain is felt over the tendons of the thumb, it is likely that de Quervain’s tenosynovitis may be present.
Non-Surgical and Surgical Treatment
The best course of treatment is determined by the severity of the condition. In conservative, non-surgical wrist pain treatment, rest and immobilization such as the use of a splint (Fig. 1) is used to prevent movement until the condition subsides. Ice, 3-4 times daily may help with the pain and swelling. Medications such as non-steroidal anti-inflammatory medications (NSAID’s) may aid in your discomfort. A corticosteroid injection is another option as it will aid in the inflammation and pain in the affected tendon sheath. Occupational or physical therapy is a useful tool in relieving pain. Your therapist will focus on reducing and eliminating the cause of irritation by promoting proper exercises and strengthening techniques to the wrist (Fig. 2-3). Typically, people notice improvement within 4-6 weeks.
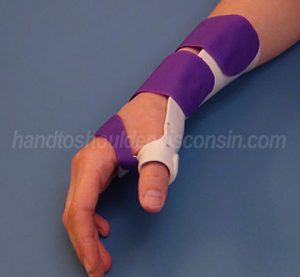 Figure 1: Immobilization splint |
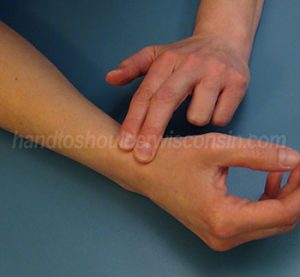 Figure 2: Transverse friction technique |
 Figure 3: Light thumb strengthening |
In severe cases, surgery may be warranted. Surgical release of the first dorsal compartment releases the tight covering of the tendons allowing the tendons room to move freely. This surgery is performed as an outpatient procedure and can be performed at Woodland Surgery Center, adjacent to Hand to Shoulder Center of Wisconsin or at one of the three local Fox Valley hospitals.
Rehabilitation is often required after surgery and is an important part of your recovery. Occupational or physical therapy sessions typically proceed for 6-8 weeks; concentrating primarily on strengthen and stabilizing the muscles and joints in the wrist and thumb.